Overview
This article highlights the critical need to identify and respond to the signs of dehydration in elderly individuals, a concern that can profoundly affect their health and well-being. Recognizing symptoms like dry mouth, confusion, fatigue, and dark urine is essential. Caregivers play a vital role in promoting hydration, and this article offers supportive guidance on increasing fluid intake and monitoring strategies to prevent severe health complications.
In addition, understanding these signs can help caregivers take proactive steps to ensure their loved ones remain healthy and comfortable. The journey towards better hydration starts with awareness and compassion. We encourage caregivers to stay vigilant and attentive, as their support is crucial in maintaining the well-being of the elderly.
Furthermore, by fostering open communication and encouraging regular fluid intake, caregivers can create an environment that prioritizes hydration. Remember, your comfort and health are our priorities, and we’re here for you every step of the way. Together, we can make a difference in the lives of those we care for.
Introduction
Recognizing the signs of dehydration in elderly individuals is crucial. This often-overlooked condition can lead to serious health complications, affecting up to 40% of seniors. Awareness and timely intervention can make a significant difference in their well-being. Caregivers and family members may feel uncertain about how to effectively monitor hydration levels and respond to symptoms. This raises an important question: what are the key indicators of dehydration that should not be ignored?
In this article, we will delve into the ten critical signs of dehydration in the elderly. Our goal is to equip you with the knowledge needed to identify and address this potentially life-threatening issue. Remember, your loved ones’ comfort and health are our priority, and we’re here to support you in this journey.
Best Care Nurses Registry: Expert In-Home Care for Dehydration Management
Best Care Nurses Registry, a family-owned and trusted home health care provider since 1980, specializes in personalized care for seniors. We understand the unique challenges that older adults face, particularly the signs of dehydration in elderly, which can affect up to 40% of this population. This condition can lead to serious health issues such as confusion, fatigue, increased risk of falls, kidney infections, and signs of dehydration in elderly patients. Our dedicated team of registered nurses and caregivers is committed to preserving independence and enhancing quality of life through effective fluid management strategies tailored to individual needs, particularly during hot weather or illness.
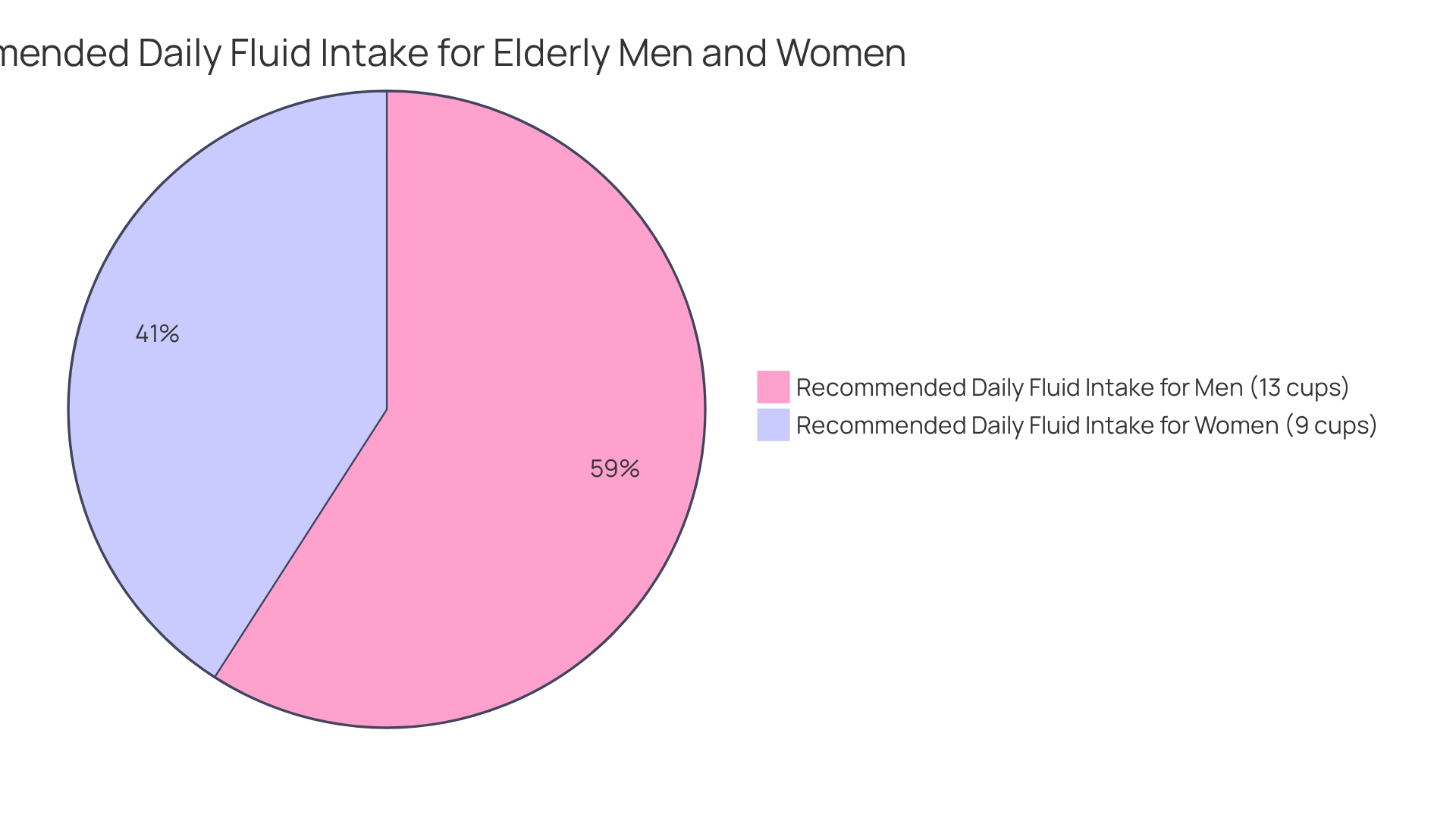
To address the signs of dehydration in elderly individuals, our caregivers encourage them to increase their liquid intake. They do this by presenting water-laden foods and drinks and ensuring that beverages are readily available throughout the day. We also take the time to inform families about the importance of maintaining fluid intake to avoid signs of dehydration in elderly, especially since the sensation of thirst naturally diminishes with age. This can lead to older adults being less aware of their fluid needs. As a guideline, we recommend a daily fluid consumption of:
- 13 cups for men
- 9 cups for women
By fostering an environment that prioritizes fluid intake, Best Care ensures that elderly individuals receive the essential assistance they need to remain healthy and active. Together, we can make a difference in the lives of our seniors, ensuring they feel cared for and supported every step of the way.
Dry Mouth: A Key Indicator of Dehydration in Seniors
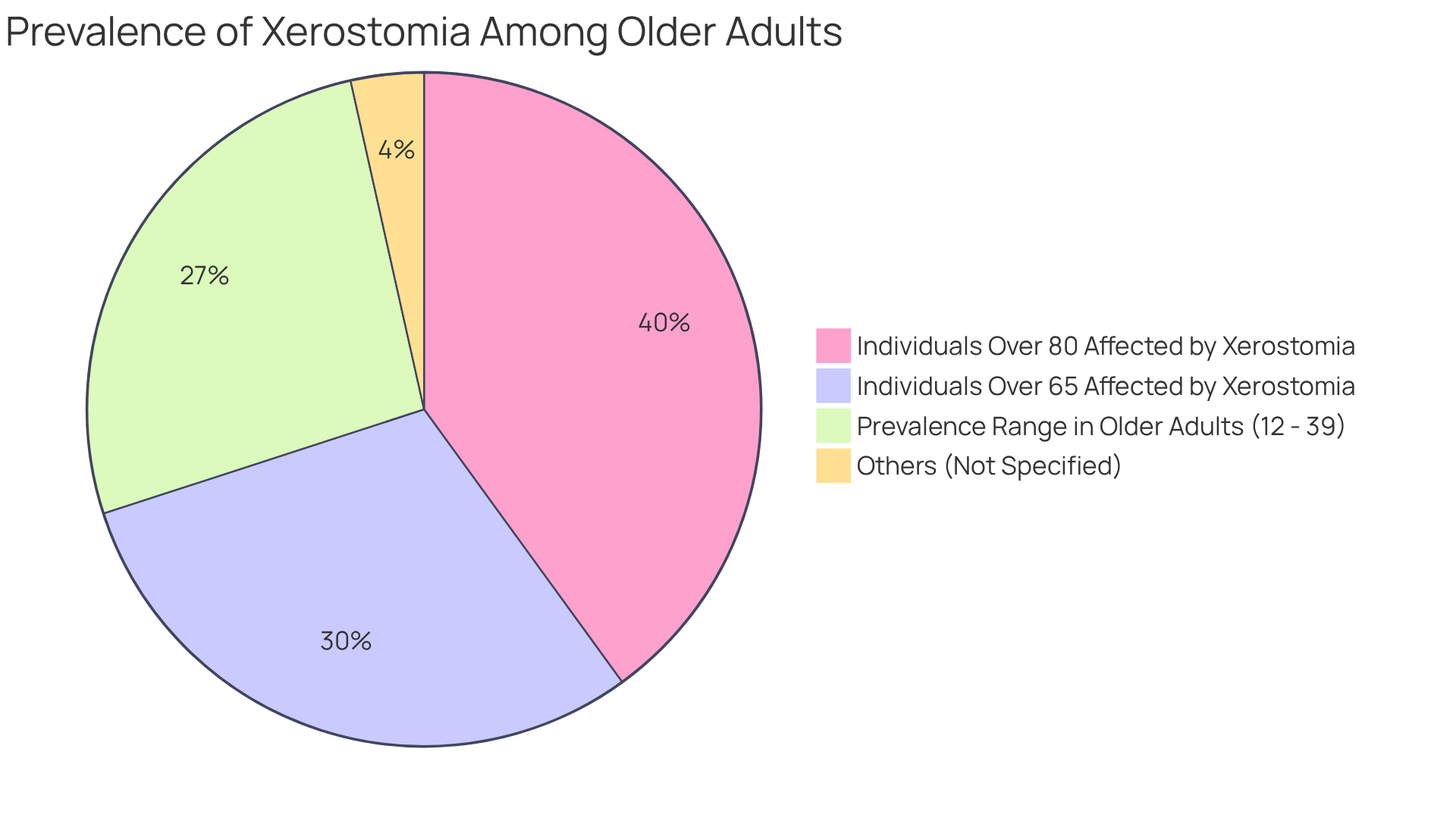
Dry mouth, clinically known as xerostomia, can be quite uncomfortable and challenging, especially for our seniors. It occurs when salivary glands do not produce enough saliva, leading to difficulties in swallowing. This condition is notably prevalent among older adults and often serves as one of the signs of dehydration in elderly. Did you know that xerostomia affects around 30% of individuals over 65? Prevalence estimates for this condition range from 12% to 39% in older adults and can escalate to 40% in those over 80. It’s essential for caregivers to be vigilant in monitoring signs of dehydration in elderly individuals, particularly those who may struggle to communicate their thirst effectively.
Furthermore, it’s important to note that patients taking one or more medications daily are twice as likely to experience xerostomia compared to those who do not take any medication. Recent studies have underscored the connection between xerostomia and fluid levels, highlighting that inadequate saliva production can significantly impair oral health. This can increase the risk of dental caries, periodontal disease, and overall well-being.
Understanding the implications of dry mouth is crucial for timely intervention. By being aware and proactive, we can help maintain hydration and comfort for our older adults and recognize the signs of dehydration in elderly. Remember, your role in monitoring these symptoms is vital, and we’re here to support you every step of the way.
Fatigue and Weakness: Warning Signs of Dehydration in Elderly Adults
Fatigue and weakness in elderly adults often manifest as diminished energy or increased lethargy, which can easily be mistaken for the natural aging process. However, these symptoms may signal signs of dehydration in elderly individuals, a condition that significantly impacts energy levels and affects 20% to 30% of older adults. It’s essential for caregivers to remain vigilant for any noticeable changes in their loved ones’ energy and to encourage regular beverage intake when such signs are observed.
Older women are recommended to drink at least 1.6 liters of fluids per day, while older men should aim for at least 2 liters. To combat fatigue, consider providing hydrating foods such as watermelon and soups. Utilizing visually appealing water bottles and planning reminders for fluid intake throughout the day can also be helpful. Furthermore, creating a supportive environment where seniors feel comfortable discussing their hydration needs can enhance their overall well-being.
Recognizing the difference between typical aging and signs of dehydration in elderly is crucial. While some tiredness is expected with age, persistent fatigue should not be overlooked; it may indicate a need for increased water consumption or medical advice. Caregivers should also be attentive to signs of dehydration in elderly individuals, which include severe fluid loss symptoms such as:
- Dark-colored urine
- Dizziness
- Confusion
These can lead to serious consequences like an increased risk of falls and urinary tract infections. Remember, we’re here for you, and your loved one’s comfort is our priority.
Medication Side Effects: A Contributing Factor to Dehydration in Seniors
Medications such as diuretics and laxatives can significantly increase liquid loss, raising the risk of severe thirst in older adults. It’s important for caregivers to be attentive to the medications prescribed to their clients, especially when multiple prescriptions are involved. Research indicates that 40% to 66% of elderly individuals show signs of dehydration, often exacerbated by medications that promote moisture loss. For instance, diuretics like furosemide (Lasix) and lisinopril (Zestril), commonly used to manage conditions such as high blood pressure, can lead to increased urination and thirst. Similarly, laxatives may draw water into the intestines, further compounding fluid loss.
To effectively monitor hydration levels in older patients on diuretics, caregivers should:
- Regularly assess liquid intake and urine output.
- Observe urine color as a quick indicator of hydration status; pale yellow urine typically reflects adequate hydration, while dark urine may signal dehydration.
- Encourage clients to drink fluids throughout the day, enhancing the palatability of water by adding flavors to make it more appealing.
Pharmacists emphasize the importance of consulting healthcare providers when medications are suspected to contribute to fluid loss. Dr. Sanjay Kurani notes, ‘Blood pressure medications such as diuretics are commonly associated with signs of dehydration in elderly patients.’ Caregivers should routinely review medication plans to identify potential side effects and adjust fluid intake as necessary. With approximately 46% of community-dwelling individuals aged 57 to 85 taking both prescription and over-the-counter medications, being aware of these interactions is crucial for maintaining fluid balance and overall health in the elderly.
Moreover, caregivers should recognize barriers to beverage consumption, such as social anxieties and mobility challenges, which can hinder older adults from consuming enough liquids. To support hydration efforts, caregivers can:
- Set reminders for fluid intake.
- Offer flavored water to encourage drinking.
Remember, your comfort and well-being are our priority, and together we can ensure that hydration remains a vital part of your daily care.
Confusion and Disorientation: Cognitive Symptoms of Dehydration in the Elderly
In elderly individuals, signs of dehydration can significantly impair cognitive function, leading to confusion and disorientation that may closely resemble symptoms of dementia. This overlap makes it essential for caregivers to accurately differentiate between the two conditions. The signs of dehydration in elderly individuals, such as dizziness, fatigue, and cognitive decline, can often be mistaken for dementia-related issues. For instance, older adults may show signs of dehydration in elderly individuals, such as increased forgetfulness or difficulty concentrating, which can exacerbate concerns about their cognitive health.
Research indicates that even mild fluid loss can lead to cognitive impairments, affecting attention and memory. In fact, a meta-analysis discovered that a decrease of merely 2% in body mass caused by fluid loss can significantly impair executive function and motor coordination. Additionally, older individuals are especially susceptible to fluid loss, and this can manifest as signs of dehydration in elderly, with research indicating that they are 20% to 30% more likely to experience this issue due to factors such as reduced thirst sensation and ongoing health problems. The prevalence of fluid deficiency in community-dwelling older adults ranges from 1% to 60%, highlighting the widespread nature of this issue.
Neurologists emphasize the critical role of hydration in maintaining cognitive health. Consistent fluid consumption is essential for avoiding the cognitive signs linked to a lack of water, which can involve heightened confusion and mood alterations. Betsy Mills, PhD, observes that the brain grows less responsive to the thirst indicator as one ages, making it difficult for caregivers to identify a lack of hydration. Caregivers should be vigilant in monitoring hydration levels, as early recognition of signs of dehydration in elderly individuals can mitigate the risk of dehydration-related cognitive decline.
Ensuring that elderly individuals consume adequate fluids—approximately 2.0 to 2.7 liters for women and 2.5 to 3.7 liters for men daily—can help maintain their cognitive function and overall well-being. Furthermore, tackling fluid loss is vital not only for well-being but also for alleviating the financial strain on healthcare systems, as fluid loss plays a major role in hospital admissions and related expenses. Remember, we’re here for you, and your comfort is our priority.
Chronic Illness and Mobility Issues: Risk Factors for Dehydration in Seniors
Elderly individuals with long-term health conditions, such as diabetes and heart disease, along with those facing mobility challenges, are particularly vulnerable and may show signs of dehydration in elderly. Did you know that seniors over the age of 85 are three times more likely to exhibit signs of dehydration in elderly, which can lead to hospitalization due to fluid deficiencies compared to their younger counterparts? This alarming statistic highlights the importance of hydration, as the signs of dehydration in elderly individuals contribute to a 6% increase in hospitalizations each year. This issue is often exacerbated by difficulties in obtaining liquids and a diminished ability to recognize thirst, both of which can contribute to the signs of dehydration in elderly.
As caregivers, your role is vital in mitigating these risks. Ensuring that water is always accessible and encouraging regular beverage intake throughout the day can make a significant difference. Consider implementing strategies like:
- Setting reminders for hydration breaks
- Providing a variety of fluid options
- Incorporating hydrating foods into meals
These simple actions can greatly enhance fluid consumption.
Moreover, it’s essential to be vigilant for signs of dehydration in elderly individuals, including symptoms like fatigue, confusion, and dark-colored urine. These symptoms can escalate quickly in seniors with mobility issues. Importantly, over 50% of older adults on diuretics experience fluid loss, underscoring the need for caregivers to be particularly attentive to this group. By prioritizing fluid intake and being observant of the signs of dehydration in elderly individuals, you can help maintain their health and well-being, ultimately reducing the risk of serious complications related to dehydration.
Remember, establishing regular fluid intake plans can significantly impact the lives of older adults. We’re here for you, and your comfort is our priority.
Encouraging Fluid Intake: Effective Strategies for Caregivers
Caregivers play an essential role in promoting hydration among older adults by applying a range of effective approaches. Offering a diverse selection of beverages, such as water, juice, and flavored options, can significantly enhance the appeal of drinking. Did you know that research suggests elderly individuals often intake inadequate liquids? In fact, studies reveal that 85.5% of older adults fail to meet daily water intake guidelines, and 88% of residents aged 85 and above consume less than 1500 mL/day. To address this concern, caregivers can set gentle reminders for seniors to drink regularly, seamlessly incorporating fluid intake into daily routines. For instance, serving water with meals or providing flavored water can make the experience more enjoyable.
In addition, caregivers should actively monitor fluid intake and be prepared to adjust their strategies based on individual needs. Methods like utilizing high-contrast drinking containers can enhance visibility and promote consumption. Furthermore, providing beverages during social gatherings can foster a more welcoming environment for drinking. Technology, such as mobile apps and smart water bottles, can also assist caregivers in tracking hydration levels and sending timely reminders to seniors.
By encouraging a setting that emphasizes fluid consumption, caregivers can help reduce the dangers linked to a lack of hydration, which can lead to severe health issues, such as cognitive decline and higher mortality rates. As Monique Ferry notes, “The prevention of dehydration must be multidisciplinary.” Ultimately, an active strategy for fluid intake not only supports the physical well-being of older adults but also improves their overall quality of life. We encourage you to think about utilizing a water tracking application to oversee liquid consumption and establish reminders for elderly individuals.
High-Water Content Foods: Nutritional Support Against Dehydration
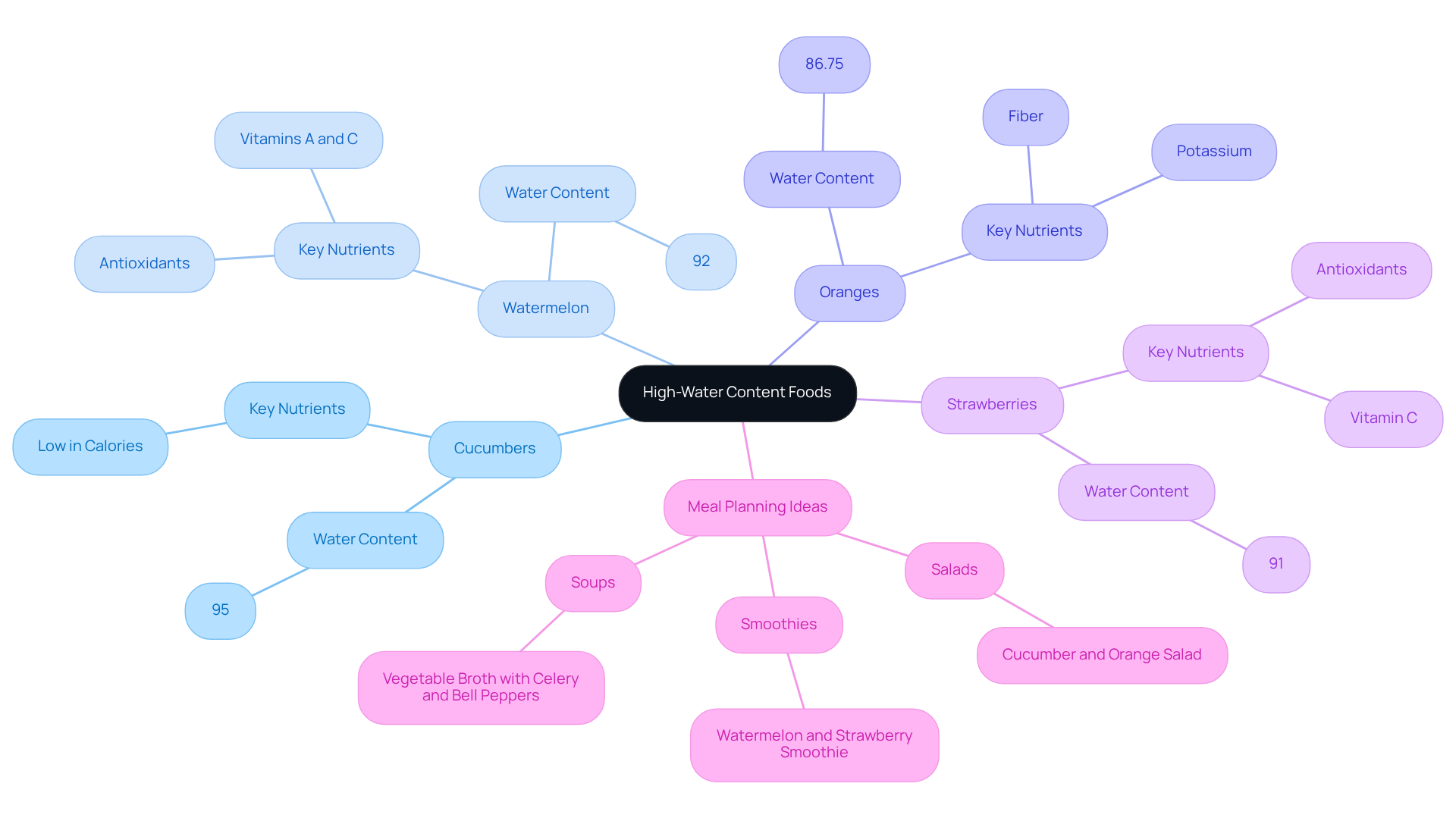
Foods high in water content, such as cucumbers, watermelon, and oranges, play a vital role in helping seniors maintain adequate fluid levels. These hydrating foods not only contribute to fluid intake but also provide essential nutrients that support overall health. Did you know that cucumbers are made up of approximately 95% water? This makes them an excellent choice for staying hydrated. Watermelon, with its 92% water content, is not only refreshing but also packed with vitamins A and C, along with antioxidants. Oranges, offering nearly half a cup of water each, are rich in fiber and potassium. Furthermore, strawberries, consisting of about 91% water, are nutritious and make a delightful addition to smoothies.
To effectively incorporate these foods into a senior’s diet, caregivers should aim for a diverse selection of hydrating options. Meal planning can include:
- Refreshing salads featuring cucumbers and oranges
- Smoothies made with watermelon and strawberries
- Soups and broths enriched with vegetables like celery and bell peppers
Soups and broths, primarily made of water, can be enhanced with extra vegetables for added moisture. By incorporating these high-water content foods into daily meals and snacks, caregivers can significantly improve moisture levels and nutritional support for the elderly, thereby helping to address the signs of dehydration in elderly individuals and ultimately promoting better health and well-being.
It is also important to encourage seniors to drink water alongside these hydrating foods to ensure thorough moisture. As specialists highlight, maintaining sufficient beverage consumption is crucial for overall health, particularly to avoid signs of dehydration in elderly adults. Remember, your comfort and well-being are our priority, and we’re here to support you in making these nourishing choices.
Regular Monitoring: Essential for Preventing Dehydration in Seniors
Caregivers play a vital role in ensuring that elderly clients maintain adequate moisture levels. By consistently tracking beverage consumption and being attentive to signs of dehydration in elderly individuals, caregivers can make a significant difference in their clients’ health. It’s essential to encourage elderly individuals to drink throughout the day, as many do not feel the natural thirst that prompts them to hydrate.
Keeping a record of water intake can be an invaluable tool for monitoring daily beverage consumption. This enables caregivers to identify trends that may indicate signs of dehydration in elderly individuals. Did you know that fewer than 15% of hospitalized older patients meet the recommended daily beverage intake of at least 1.7 liters? Organized monitoring methods can greatly enhance water intake among elderly individuals, leading to better health outcomes.
By utilizing fluid tracking records, caregivers can ensure that elderly individuals receive the necessary liquids, ultimately supporting their overall well-being. Educational initiatives have highlighted the importance of hydration assessment techniques, reinforcing that regular checks and documentation can lead to improved outcomes for our cherished older adults. This proactive approach not only helps prevent fluid loss but also fosters a nurturing environment where older adults can thrive. Remember, your comfort and health are our priority, and we’re here for you every step of the way.
When to Seek Medical Help: Recognizing Severe Dehydration Symptoms
Severe fluid loss can pose significant health risks, including kidney failure and shock, especially for older adults. It’s concerning to note that 17-28% of older adults in the United States are chronically dehydrated. This reality makes it crucial for caregivers to remain vigilant. If a senior exhibits signs of dehydration in elderly, such as:
- Extreme thirst
- Dry mouth
- Confusion
- Very dark urine
- Inability to retain fluids
seeking medical assistance should be a priority. These symptoms are signs of dehydration in elderly individuals, indicating a critical state that requires prompt intervention to prevent further complications.
Emergency care experts emphasize that timely medical intervention can be life-saving. Fluid loss can lead to severe complications, including organ damage. As Samruddhi Yardi points out, “Severe fluid loss can lead to organ damage and other serious complications.” Regularly monitoring hydration levels is essential for maintaining the health and well-being of seniors, particularly during hot weather or illness. Signs of dehydration in elderly individuals are a frequent cause of hospital admissions among this population, and your comfort is our priority. Let’s work together to ensure that our loved ones stay hydrated and healthy.
Conclusion
Recognizing the signs of dehydration in elderly individuals is crucial for their overall health and well-being. It’s important to remain vigilant about hydration, especially since older adults often experience diminished thirst sensations and face various health challenges that heighten their risk of dehydration. By understanding the symptoms and implementing effective strategies, caregivers can play a vital role in ensuring seniors maintain adequate fluid levels.
The prevalence of dehydration among older adults is concerning. Medications can impact hydration, and the cognitive effects of dehydration, such as confusion and disorientation, can be alarming. Furthermore, practical strategies for promoting fluid intake—like incorporating high-water content foods and regularly monitoring hydration levels—are essential. These measures not only help prevent severe health complications but also enhance the quality of life for seniors.
In conclusion, prioritizing hydration in elderly care is essential. Caregivers are encouraged to adopt proactive measures to monitor fluid intake and recognize the signs of dehydration early. By fostering a supportive environment that emphasizes the importance of hydration, we can significantly improve the well-being of older adults. Taking these steps can lead to healthier, more active lives for seniors, ensuring they receive the care and attention they deserve.
Frequently Asked Questions
What is Best Care Nurses Registry?
Best Care Nurses Registry is a family-owned home health care provider that has been in operation since 1980, specializing in personalized care for seniors, particularly in managing dehydration.
Why is dehydration a concern for the elderly?
Dehydration can affect up to 40% of older adults and can lead to serious health issues such as confusion, fatigue, increased risk of falls, and kidney infections.
How does Best Care Nurses Registry help manage dehydration in elderly individuals?
The registry encourages increased liquid intake by providing water-laden foods and drinks, ensuring beverages are readily available, and educating families on the importance of hydration.
What is the recommended daily fluid intake for elderly individuals?
The recommended daily fluid consumption is 13 cups for men and 9 cups for women.
What is dry mouth, and how is it related to dehydration in seniors?
Dry mouth, or xerostomia, is a condition where salivary glands do not produce enough saliva, making it difficult to swallow. It affects around 30% of individuals over 65 and serves as a key indicator of dehydration.
How prevalent is xerostomia among older adults?
Xerostomia affects approximately 12% to 39% of older adults, escalating to 40% in those over 80.
What factors increase the likelihood of experiencing dry mouth in seniors?
Seniors taking one or more medications daily are twice as likely to experience xerostomia compared to those who do not take any medication.
What symptoms should caregivers monitor for signs of dehydration in elderly adults?
Caregivers should watch for symptoms such as fatigue, weakness, dark-colored urine, dizziness, and confusion.
How can caregivers encourage hydration in elderly individuals?
Caregivers can encourage hydration by providing hydrating foods, using visually appealing water bottles, setting reminders for fluid intake, and creating an environment where seniors feel comfortable discussing their hydration needs.
What should be done if persistent fatigue is observed in an elderly person?
Persistent fatigue should not be overlooked as it may indicate a need for increased water consumption or medical advice.